Photos - Day 3 vs. Day 5 Embryos
The sequence shown below shows an 8-cell embryo on day 3 (#1) in which the cells are beginning to press up against one another (see 2 cells flattening against each other). After about 16 hours, the cells have divided again to produce a 16-cell embryo (#2) and they have compacted together even more. By day 4 of life (#3) the embryo is completely compacted to the point that individual cells can no longer be seen. At this stage the embryo is called a morula from the Latin for mulberry. The compaction process results in a fluid tight seal between cells and the embryo can now pump fluid into the center of the ball of cells. The cavitating morula (#4) also allocates cells to the inside and outside (#5) of the growing cavity or cyst. The outer cells will form the placenta of the implanting embryo and the inner cells will form the embryo proper or fetus, as well as some of the extraembryonic membranes such as the yolk sac. When the cyst is formed and cells have been allocated, the embryo is called a blastocyst (#6). The quality of a blastocyst is determined by the number of cells in the outer and inner populations as well as the degree of expansion of the cyst. 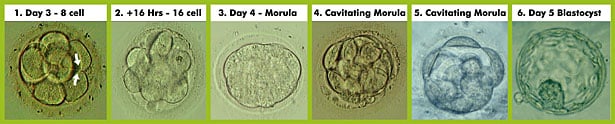
Categories
About the Blog
Welcome to the Pacific Fertility Center Blog! Nationally and internationally recognized for providing exceptional reproductive care, our team believes in empowering people with the knowledge they need to navigate their unique fertility journeys.
From information on the latest fertility treatments to valuable insights on egg donation, surrogacy, and everything in between, the Pacific Fertility Center Blog is your ultimate resource for all things reproductive care and support. Read on to learn more, and contact us today if you have any questions or want to schedule a new patient appointment.

